Â
“Pop” and your knee swells up.  You are worried because you have never felt this before to your knee.  Your knee does not feel right and it hurts to put weight on it.  The worst thoughts run through your head a mile a minute.  Do I need surgery?  What just happened and will I be okay?  Let me reassure you that this knee experience is all too common and things will be okay.  The medical lab scientists and clinicians are so intrigued with the ACL, such that there are tons of research studies advancing the care of this popular knee ligament.  This article is a continuation of “ACL 101: the Breakdown of How Not to Break Down (The What?!)”  and will dive into the self care of an ACL rehabilitation after surgery. Are you ready to get “science nerdy” to master your ACL?
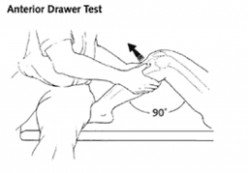 How to know if you have an ACL tear?
How to know if you have an ACL tear?
The are two simple tests: the anterior drawer test and Lachman test.  Both tests are done by cupping the shin bone and shifting it forward.  One test the knee is at 90 degrees and other at 30 degrees, respectively.  The goal is to feel if there is any difference to the uninjured knee.  These tests are used after injury and during rehab care to understand the sturdiness of the ACL.
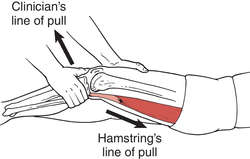 A “looseness” indicates that the ACL is impacted, either sprained or torn. Â If the knee is swollen then you might not get accurate result. Â The ACL test has two parts and each test assesses the individual parts. Â The recovery care does not change based on what parts are injured. Â Us medical nerds likes to get technical.
A “looseness” indicates that the ACL is impacted, either sprained or torn. Â If the knee is swollen then you might not get accurate result. Â The ACL test has two parts and each test assesses the individual parts. Â The recovery care does not change based on what parts are injured. Â Us medical nerds likes to get technical.
History of ACL care and rehab paradigm/methods
If you are a “why this” person, understanding the history will allow you to appreciate your knee care. Â ACL care in the 80’s and 90’s was dependent on tissue understanding and applying it to rehab care. Â Ligaments takes forever to “heal” so everyone was overly cautious. Â An ACL surgical ligament takes two years to “heal”. Â We braced and limit movement of the knee. Â This short term “nervousness” impacted the knee’s long term “health” because it led to a lot of stiff knees resulting in osteoarthritis and other compensatory ailments.
The pendulum shifted in the opposite and rehab care was about ego and bragging rights. Whoever could get this athlete better faster is the “man.”  This ideology led to osteoarthritis because the knee was not ready to handle high loads.  The model of rehab in the 2000’s was more isolated by design and this was a flaw.  The human body is a powerful machine when everything works together with each other.
Here we are in the 22nd decade where ACL rehab is in the middle. Â Surgical technology is more advanced and rehab is more integrative. Â The design has a better understanding of not being overprotective but not too rushed.
What to expect after having ACL surgery?
Early movement and progressive weight bearing to your leg are key after ACL surgery. There will be no honeymoon period where you knee gets to relax and chill. Â Your knee will be braced to protect your swollen knee. Â The use of your brace is dependent on the philosophy of your surgeon. Â The efficacy of it is that bracing is good for short term but no extra benefit long term. Â Swelling will be your biggest enemy during this whole recovery experience. Â Studies have demonstrated that fluid as little as the size of a bottle cap can shut down your front thigh (quadriceps) muscle. Â This will result in a giving out sensation, hence the brace for the initial 4-6 weeks after surgery and before surgery. Â If you brace your knee hard enough you may compensate but at a higher energy cost to your body. Â In summary, ice and compress your knee for 20 minutes 4-6 times a day for the first 3 months after surgery. Â After you ice your whole knee, one may feel the surgery scar being warm. Â Get an ice cube and rub it over the warm spots until that is cold.
Your next biggest enemy is anterior thigh (quadricep) weakness. Â I mentioned above that strength is dictated by swelling. Â Multiple studies have shown that short and long term success and aging gracefully at your knee is dependent on this muscle. Â An important milestone and exercise focus is to regain your ability to sustain a quadricep contraction for one minute without any shaking feeling. Â The sooner the better is the saying. Â I can progress but usually will not advance any ACL program if this milestone is lacking. Â This phenomenon of quadricep strength can also dissappear anytime during your recovery, so do not deemphasize this exercise. Â There are many exercises that I have developed that challenge this specific ability of the quadriceps to sustain a strong hold. Â The ability to achieve this milestone varies from individual. Â Do not panic if you have trouble achieving this milestone because month 2 to 3 is when the ACL repair is at its weakest. Â The first 3 months is where I like to focus on the basics because we want to respect our body to heal well for the long run. Â Electrical stimulation should be used early on to assist with muscle activation.
The purpose of the first 3 months is to regain strength and control of your lower body. Â This is where I believe many ACL rehab can separate itself from good to great care. Â My next milestone is to ensure that your core is rebalanced for the next phase (3 months and on) of recovery. Â If you read “How to Build A Superhuman (The ReVITALize Way)” I wrote about the importance of our internal organs impacting our outer core. Â Our outer core is comprised of a group of deep muscles including our diaphragm, pelvic floor, obliques, hips and deep abdominals. Â I have a strict screen that indicates if one’s core has the ability to work with your limbs (legs) and sufficient capacity to build strength upon it. Â This is what separates many recoveries apart from each other. Â Many assume that the core is helping the legs without any way of measuring and confirming. Â Many assume that if there is no pain with core exercises that the program is fitting for the client. Â This is where I tend to not budge and will try every methodology and tricks to not sacrifice this milestone. Â It is not uncommon for me to address dysfunctions to the internal organs which will “wake up” the outer core. I will use this screen every week to “check in” with the core and advise this should be a new habit when working out.
“Neuroreflexive” Core screen criteria (need to achieve all three to pass)
- Deadbug (Isometrics) Hold of 30 seconds
Position: Lay on your back and raise your arms and legs up.  Hips and knee angle           should be at a  90-degrees.  Arms should be reaching up towards the ceiling, palms         facing inwards.  Ankles should be aligned with you shoulder and knees.
Test: The act of you being in this position should cause you to feel your abdominals         working ONLY.  NO low back, groin, front leg muscles should be felt.
    2. Bridging (Isometrics) Hold of 60 seconds
Position: Lay on your back and raise your hips and chest up high as you can.  Feet hips      width apart.  Hands firmly to your side.
Test: The act of you being in this position should cause you to feel your gluteals (rear)Â Â Â Â Â Â Â working ONLY. Â NO low back, groin, front leg muscles should be felt.
    3. Side Leg Lifts (Isometrics) Hold of 30 seconds
Position: Lay on your side with your shoulder/back/leg against the wall.  Slide your         leg about two feet up.  Hold.
Test: The act of you being in this position should cause you to feel your side gluteals      (where your side buttock dimple is at…or the side border of your back pocket)              working ONLY.  NO low back, groin, front leg muscles should be felt.
The next part of this ACL series is to help one trying to avoid ACL surgery. Â The key is to teach yourself how to a “coper.” Â Train the knee to act like it has an ACL ligament and do it well. Â If you are having ACL surgery or have general knee questions, contact us with them for an expertise advice. Â If you want to improve on moving and exercising more but do not know where to start because of pain, we provide services to structure a fitness program based on your desired goal.
Contact us for my actual program that my clients go through during their first 4 months of ACL recovery. This program will be broken down into specific criterion and will allow you to gauge where you are at in your own recovery.
photo credit:http://www.gannett-cdn.com/-mm-/ac1394dbdcca6a36cbf486633b129cd813095ac3/r=x404&c=534×401/local/-/media/USATODAY/USATODAY/2012/12/06/adrian-peterson-12-07-12-4_3.jpg

